Who: Drs. Khan and Wallace
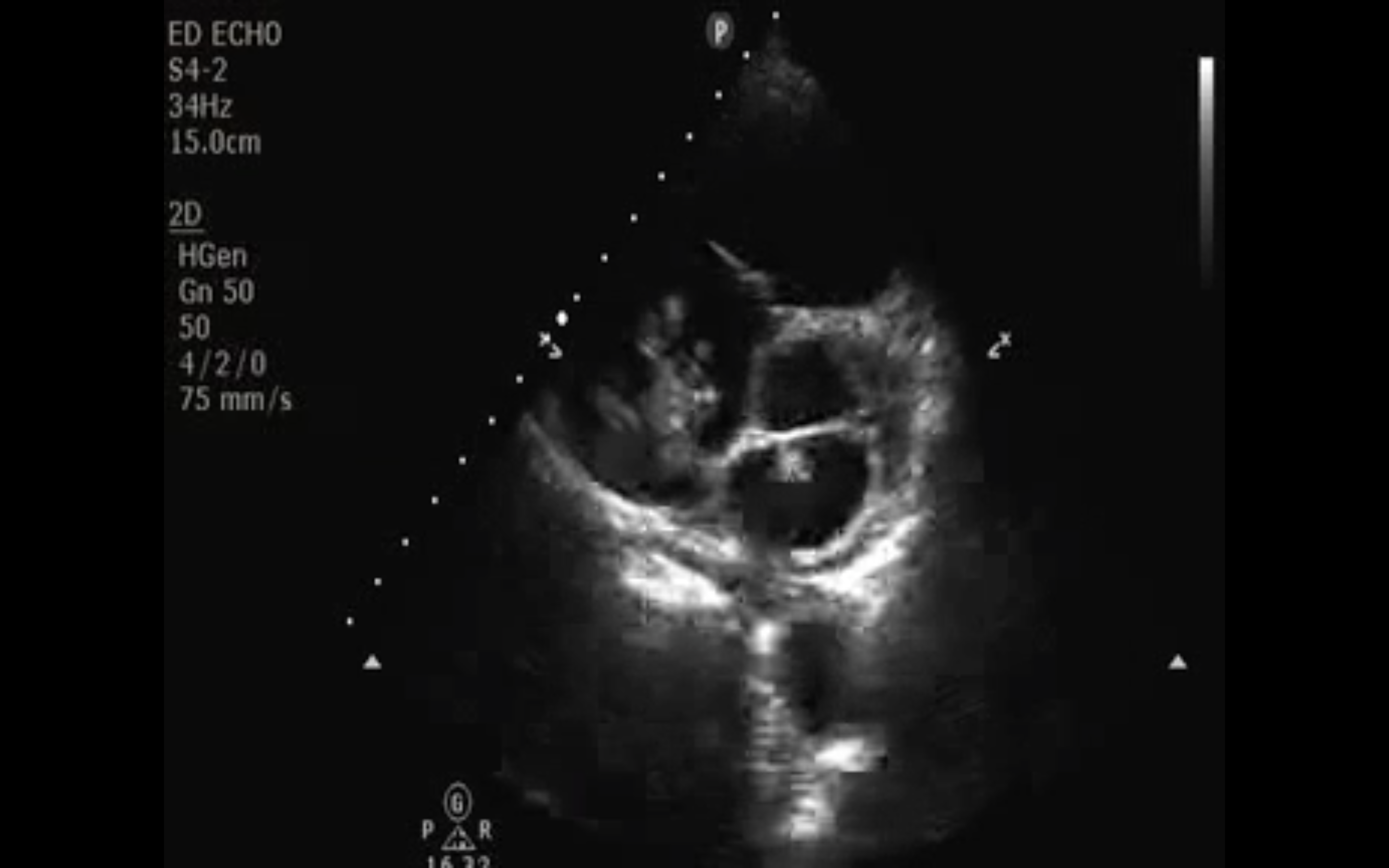
Through a bedside echo, the dynamic intern duo diagnoses a large right atrial thrombus. Further close inspection of the video shows the patient has a PFO and clot can be seen moving between the right and left heart. The clot in the right heart can be seen in patients with pulmonary embolus (PE). Remember PEs start as DVTs. Then they travel through the IVC and the right heart, finally lodging in the pulmonary arteries. Drs. Khan and Wallace also used ultrasound to demonstrate right heart strain and the cardinal signs of PE.
ED bedside echo minimally comprises three views: subxiphoid, parasternal, and apical 4-chamber. Pericardial effusion, ejection fraction evaluation, and chamber enlargement are best assessed in the subxiphoid, parasternal, and apical 4-chamber views, respectively. Intra-cardiac clot, however, may be visualized in any view. Depending on clot acuity, the appearance may be hyper (bright) or hypo (darker) echoic.
Image 1
This may be a review, but here is how to obtain the different heart views:
Subxiphoid view: Place the probe with a probe marker pointing to the patient's right side, midline in the subxiphoid space.
Parasternal view: Place the probe in the fourth intercostal space, just left of the sternum with the probe marker pointed to the patient’s left hip. Rotating the probe 90 degrees visualizes the heart in its short axis. When transitioning from the parasternal long view, simply rotate the probe marker from the left hip to the right hip.
Apical-4 chamber view: Place the probe with a probe marker oriented to the patient right at the point of maximal impulse (PMI).
Deep venous thrombosis may be visualized on ultrasound by the presence of an intraluminal clot and/or incomplete venous wall coaptation under pressure. ED bedside ultrasound detection of pulmonary embolism, however, is an indirect assessment; we may not simply assess pulmonary vasculature using ultrasound. Rather, clinically significant pulmonary embolism is detected through ultrasound confirmation of right heart strain. Right ventricular enlargement, along with the “D” and McConnell’s signs, are ultrasonographic surrogates of right heart strain.
The healthy right ventricle is two-thirds the size of its left counterpart. Right heart strain, however, results in right ventricular dilation with the ventricle appearing as large or even larger than the left ventricle.
The D-sign is located in the parasternal short-axis view. Healthy hearts have a large circular left ventricle with a much smaller right ventricle in this view. Right heart strain leads to a larger right ventricle compressing the left ventricle during systole. The left ventricle appears shaped like a capital “D”.
Right heart strain may lead to wall motion abnormalities. McConnell’s sign is simply an akinetic free wall of the right ventricle with sparing of the apical section. This is the only sign that is specific for PE.
Clinical Importance: It can be extremely helpful to perform a rapid cardiac ultrasound in unstable patients. In patients with hemodynamic dysfunction, dyspnea, and/or chest pain, the differential diagnosis can be quickly narrowed at the bedside. Understand and learn to rapidly perform all views because, in isolation, one view may only answer one question. The heart is a three-dimensional structure and anyone two-dimensional ultrasound view only solves a part of the clinical conundrum. In combination, the three views resolve focused clinical queries.
The lodged clot in the right heart should immediately make you think about large PE. These patients may benefit from IR or surgical consultation for catheter-directed thrombolytic or thrombectomy.
It is also important to note that right ventricular enlargement and the D sign may also be present in patients with chronic right ventricular strain, such as patients with pulmonary hypertension, and may not be specific for pulmonary embolism. While bedside echo may reveal definitive signs of pulmonary embolism as described, diagnostic accuracy is increased with combination ultrasonographic evaluation of the lungs, lower extremities, and IVC.
PFOs are not typically large enough to be easily seen on bedside US. They are typically diagnosed with a bubble study, or by using color Doppler to identify flow across the atrial septum in the subxiphoid view.
Date: November 2013
